Price Transparency in Healthcare: Impacts on Strategy & Marketing
Tim Duer
Healthcare, Marketing
September 21, 2021
Price Transparency in Healthcare: Impacts on Strategy & Marketing
As travel restrictions have continued to lift over the past 12 months, it seems like everyone is thinking about their next vacation. After months of hardly getting to leave home, who can blame anyone. Imagine if you planned a dream trip, hopped on an airplane, stayed at a great hotel, enjoyed your drinks and meals and then headed back home; but didn’t know what it was going to cost until you received a bill 3 months after you returned?
While this sounds like a crazy idea, it is exactly what we’ve come to expect from healthcare in the United States. Making matters even worse, the costs of the care have often been carefully guarded negotiations between health systems and insurers, and patients often rely on the providers to tell them what they need. As a result, people have been electing to go to the hospital, undergo surgery, have some (maybe not so great) meals, and then wait for a bill to show up in the mailbox a few months later. Not only are many patients not aware of what the charges will be for services, but they also are often not aware of what healthcare services they are receiving.
Price Transparency Rule
As of January 1, 2021, the hospital Price Transparency Rule required that all hospitals make their cash and insurance negotiated rates for 300 “shoppable” services available to the public. While this appears to be a great improvement for the patients’ ability to understand their cost of care, in reality, things are not quite so simple. First, many systems have been slow to post the information or have not yet posted the information in its entirety. A June 2021 article in the Journal of American Medical Association (JAMA) reported that approximately 82% of sampled hospitals were non-compliant with at least one of the legislation’s major requirements. A second challenge is the significant variation in negotiated rates; with large disparity in charges depending on the insurer, even for the same procedure at the same hospital. A final contributor to the confusion stems from the general complexity in navigating the patient-provider-payer system to figure out what procedures are anticipated by the patient, recommended by the provider, and covered by the payer.
With 2020 being such a challenging year for healthcare systems worldwide, the American Hospital Association (AHA) has made a push to delay or reverse the implementation of the Price Transparency rules, but the requirements have remained in place. In a December 2020 letter to the Health & Human Services Biden-Harris Transition team, AHA president Richard J. Pollack stated that while hospitals wanted to provide information to patients on out-of-pocket costs, “the requirements related to the rates that commercial health insurers negotiate with hospitals is anticompetitive. Worse still, those rates will not be useful to consumers, but rather, will confuse and frustrate them”. As of this writing, litigation continues regarding the requirements and enforcement of many aspects of the Price Transparency Rule, but the large majority of its contents remain in place.
Price Versus Value
While hospitals continue to push back against the challenges associated with the transparency requirements, there are also opportunities for systems to utilize this information to their benefit. An August 2021 Causeway Solutions survey of 600 US residents found that 45% of respondents moderately or strongly agreed that health systems used revenue gains to advance the quality of care and 49% agreed that this revenue was used to support community health. Interestingly, 52% of men agreed with these statements as compared to only 35% of women. Health systems that emphasize the quality of care and overall benefits of the care that they provide have a growing opportunity to focus on the value of the services, rather than feeling the need to cut prices to compete with competitors.
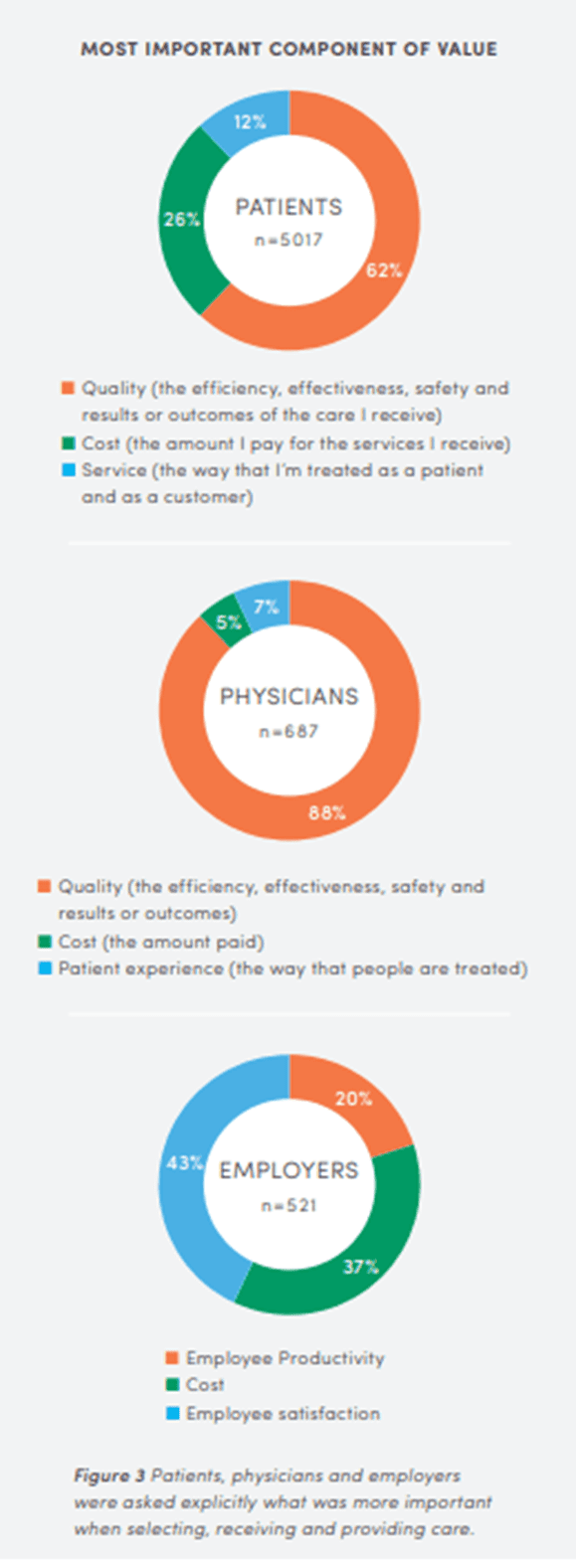
Value in healthcare (or any industry) is often defined as outcome per cost. As a result, health systems that can demonstrate better outcomes are able to promote better value for service, even when compared to competitors that have lower charges. While some consumers will certainly price shop among many competitors, most recognize that there is more to this important value equation than price alone; and this is especially true when it comes to personal health. This is apparent in a 2017 University of Utah (see sidebar) study surveying more than 5,000 patients nationwide; it found that 62% of patients felt that quality (efficiency, effectiveness, safety, and results) was the most important component of the value equation, as compared to only 26% who identified costs and 12% calling out service (the way they are treated as a patient/consumer) as the primary component of value.
With this knowledge in hand, health systems should understand that price transparency should not create pricing battles between systems but instead provide an opportunity for the best hospitals to promote their quality as a reason that their services are worth more. And so, while the pros/cons and challenges of price transparency continue to be discussed nationwide, high-quality health systems can promote the message of “you get what you pay for” and make the focus of the conversation on quality rather than price alone. Ultimately, this is (or at least should be) the goal for healthcare in our country. While cost containment is incredibly important, no one wants to cut costs at the risk of cutting the quality of care.
References
Bracken, S. et al. (2017). Bringing value into focus: The state of value in U.S. healthcare. University of Utah Health; Salt Lake City, UT.
Gondi, S., et al. (2021). Early hospital compliance with federal requirements for price transparency. JAMA Internal Medicine.
Pollack, R.J. Pollack, R.J to Brooks-LaSure, C. (2020, December 21). American Hospital Association.
Ready to learn more? Contact Causeway Solutions to get started!